Hospital Exercise Offers Stress Relief
If you had a fitness routine before cancer, chances are you’re going to want to continue during treatment on days that you’re feeling up to it.
As a runner and tennis player, my normal routine was disrupted during hospitalizations of weeks at a time, so I had to come up with something else. Whatever your sport or activity, it’s going to be pretty hard to maintain consistently during blood cancer treatment.
To back up, I almost fell off the exam table during my intake exam in early April, 2003, when I learned the plan for getting rid of my leukemia. I would have three rounds of chemotherapy, with hospitalizations lasting seven to 10 days. Then I would have rest periods at home. The last, strongest round would deplete my bone marrow. A stem cell transplant to would regenerate it.
My doctor at the Dana-Farber Cancer Institute in Boston explained that although I might go into remission after the first round (which I did), they still needed to go after leukemia cells that could be hiding. He said to imagine them as being under a carpet.
Finding new ways to relieve stress
This would definitely mess up my routine of running about 15 miles a week. And in a domino effect, the stress relief that I got from running would go out the window.
“Do they have Ativan?” I asked my doctor.
“Big jars of it,” he said.
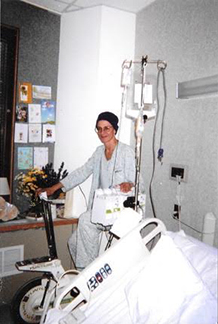
They also had an exercise bike.
My mother took a photo of me on it while I was connected to an IV pole. I didn’t exactly work up a sweat, but it felt good to be moving.
I walked with my mother and whoever was visiting (often my sister) on The Pike, a corridor connecting medical offices on a lower level at Brigham and Women’s and Hospital. At each end, I stopped to do runner’s stretches.
We also walked along The Bridge of Hope, which connects the hospital with Dana-Farber. It is decorated with birds in flight and inspiring poems by Emily Dickinson.
(At first, I thought that patients were treated at Dana-Farber, but then I learned that it consists of exam rooms, offices, clinics and outpatient treatment areas; in-patient care happens at “The Brigham.”)
One time, my nurse thought I should take a wheelchair. My sister and my mother and I piled our stuff into the wheelchair and used it as a carryall.
Coping with chemo side effects
It didn’t take long for the chemotherapy to give me diarrhea. I learned the location of all the bathrooms along our walks.
Some days I just did laps around the nurses’ station. Other patients did the same. We would stop to chat, like people walking in a park. We got to know each other. A nurse told me how many laps made a mile. Occasionally, I lifted bags of saline solution. I wasn’t a big weight lifter, but I didn’t want my arms to go to flab.
On other days, nausea, diarrhea and other complications from the chemotherapy overtook me. I curled up under the quilt that I had brought from home. I fell asleep and dreamt that I was running, my ponytail flapping in the breeze. It upset me to wake up and remember that I was bald and would not be running outside for quite a while.
Join the conversation